Osteoarthritis
Osteoarthritis
What Is Osteoarthritis?
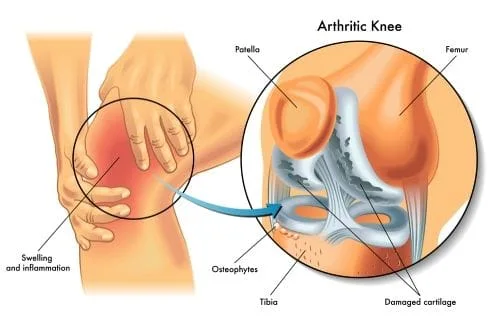
Osteoarthritis (OA) is the most common type of arthritis. It’s also referred to as “degenerative joint disease” and “wear and tear arthritis.” During osteoarthritis, cartilage begins to break down, which causes the bones within the joint to rub together and begin to wear out. This can cause pain, stiffness, difficulty moving, as well as other symptoms.
Osteoarthritis may occur in any joint in the body. However, the most common areas include:
- Hands
- Fingers
- Feet
- Knees
- Hips
- Spine
- Shoulders
Osteoarthritis is more likely to develop with age and can sometimes occur slowly over many years. It typically affects the weight-bearing joints in the body, such as the feet. While osteoarthritis develops, it can begin to affect movement and the way you walk. OA can also lead to other potential foot problems, such as bunions. It’s often aggravated by prolonged activities but relieved while resting.
Symptoms
What Are the Symptoms of Osteoarthritis?
Osteoarthritis in the foot often affects the joint at the base of the big toe and can occur in the ankle, as well as the midfoot.
The most common OA symptoms involved with the feet include the following:
- Joint pain that increases during activity
- Stiffness and swelling in the affected area
- Limited movement and flexibility in the foot
- Joint pain as a response to changes in weather
- Cracking, clicking, or popping sounds when you move your joints
- The development of bone spurs
- Other foot deformities, such as bunions and hammertoes
Causes
What Causes Osteoarthritis?
Osteoarthritis is caused by damage or degeneration to the joints. The wear and tear experienced during osteoarthritis erode the cartilage that cushions the joints. When the cartilage begins to break down, the joints rub together, which causes pain and difficulty with movement.
This is why osteoarthritis is so common with older age, as your joints have gone through repetitive stress over the years. Damages to nearby joints can accumulate over time.
The common causes of joint damages include the following:
- Increased age
- Joint deterioration
- Weakened muscles that put extra pressure or strain on your joints
- Past injuries that didn’t properly heal
- Increased weight gain can wear down the joints due to the amount of mass they have to move.
- Inactivity can lead to the weakening of muscles and weight gain, which can accelerate and increase strain on the joints.
- Specific professions that require repeated movements may lead to the development of osteoarthritis.
- Biomechanical abnormalities can misalign parts of your body. As a result, excess wear and tear can be placed on certain joints and can increase the load on your feet, ankles, or knees.
Diagnosis
How Is Osteoarthritis Diagnosed?
Unlike other arthritis pain, osteoarthritis can develop gradually over many months or years. It’s typically increased by activities that put repeated stress on your joints, such as running. As the symptoms can begin to worsen over time, it may be a good idea to see a Doctor and have it diagnosed as early as possible.
A Doctor can diagnose osteoarthritis by performing a physical exam and checking the affected area for joint pain, tenderness, swelling, and flexibility. After the physical exam, you may be tested for the following:
- X-rays: X-ray images don’t show cartilage, but they can reveal cartilage loss by examining the spaces between the bones in the joint. X-rays can also indicate whether bone spurs have formed around the joint.
- Magnetic resonance images (MRI): An MRI can produce detailed images of the bone and soft tissues, which includes cartilage.
- Blood tests: Certain blood tests can help determine what is causing the joint pain, much like with rheumatoid arthritis.
- Joint fluid analysis: A needle may be used to draw joint fluid from the affected area. The analysis can determine whether the joint pain is caused by gout or another foot condition.
Treatment
How Is Osteoarthritis Treated?
There is no cure for osteoarthritis, but the condition can be managed and treated in various ways. The most common medical treatments and recommendations for OA in the feet include the following:
- Exercises: Swimming, water aerobics, and low-impact strength training are recommended to improve joint stability, flexibility, and muscle strength.
- Physiotherapy may be recommended to strengthen and condition the affected joints and muscles.
- Proper footwear that accommodates foot deformities stemming from osteoarthritis, such as bunions or hammertoes, can decrease joint pain.
- Custom orthotics can be designed to accommodate osteoarthritis. Orthotics have control over the biomechanics that can deteriorate joints, as well as provide support and comfort to relieve pain.
- Hot and cold treatments using a heating and cooling pad or pack can provide temporary pain relief.
- Assistive devices: Braces, shoe inserts, canes, or walkers can relieve pain by keeping added pressure off your joints.
- Healthy eating or losing weight can reduce the risk of developing OA, as it will keep extra weight off of your joints.
Medications
Over-the-counter methods may be recommended as a first approach for osteoarthritis symptoms. However, there are other types of osteoarthritis medications that reduce pain, such as:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen can help with pain management and swelling.
- Oral pain relievers such as acetaminophen may help reduce pain but not swelling.
- Topical pain relievers such as OTC creams and gels will assist in numbing the affected joint area and provide relief for arthritis pain.
- Corticosteroids may be prescribed in oral form or by injection into the affected joint.
- Cymbalta, also known as duloxetine, has been FDA approved for the treatment of musculoskeletal pain.
In more advanced cases, surgeries such as joint replacement or joint fusing may be necessary.
Complications of Osteoarthritis
Any form of arthritis, especially osteoarthritis, can cause physical complications, including the following:
- Erosion of cartilage, ligaments, and tendons
- Hairline fractures
- Bleeding near the joints
- Osteonecrosis, also known as bone death
- Weight gain as a result of limited mobility
- Poor sleep due to intense pain
Risk Factors
What Are the Risks of Osteoarthritis?
While age, prior injuries or trauma, and inflammatory arthritis can cause the development of osteoarthritis, there are other factors as well.
The other risk factors of osteoarthritis include:
- Obesity: Increase in weight causes pressure and stress on your joints.
- Biomechanical abnormalities: Deviations in the foot or knee joint may cause wear and tear on certain joint locations.
- Musculoskeletal and skin diseases: These diseases can disrupt the mechanics of the body and place extra stress on your joints.
- Diabetes and hyperlipidemia can affect the inflammatory response in the body, increasing the risk of osteoarthritis.
- Gender can play a role in the development of osteoarthritis. Decreased estrogen is often experienced in post-menopausal women, which increases the risk of knee osteoarthritis.
- Heredity can factor into osteoarthritis, as those born with bone diseases or genetic traits may be more likely to develop OA.
In some cases, other forms of arthritis can cause damage to joint and muscle tissue, which accelerates the process of wear and tear.
Prevention
How Do I Prevent Osteoarthritis?
There is no concrete way to prevent osteoarthritis, as it is often related to conditional situations or age. However, there are ways that you can control or manage the factors associated with osteoarthritis.
Those helpful tips include:
- Maintaining your weight by keeping your body mass index at the appropriate range for your height, age, and sex
- Support your body by wearing supportive athletic shoes to reduce the impact on your knees. Doing so may reduce the risk of knee osteoarthritis.
- Keep active and exercise regularly to strengthen your muscles. Make sure to practice low-impact exercises in moderation with high-impact sports.
- Sticking to a nutritious diet with fruits and vegetables
- Getting the proper rest and sleep that your body requires
While there is no cure for osteoarthritis, there are various ways that it can be managed and treated. If you’re dealing with the pain associated with OA, it may be time to do something about it. At Academy Clinics, we have the proper services, treatments, and products necessary to assist you with your foot troubles. Take the first step and book an appointment with one of our skilled foot specialists today.
Meta Description: Osteoarthritis is the most common form of arthritis. It creates degeneration of the joints, causing intense pain and difficulty with mobility.